Twenty years ago, the U.S. government forced doctors to move from paper to electronic records. The result? Many doctors spend more time staring at a computer screen than they do interacting with their patients. The goal becomes inputting data, and not attempting to understand why the patient is there and what treatment plan is best for him.
This move to data-input medicine has led to doctors increasingly relying on numbers to measure patient health. I want to talk about some of these numbers, sharing my experiences and concerns.
Pain Chart
“On a scale of one to ten,” the nurse or doctor asks, “how bad is your pain?” Instead of talking to the patient about his pain, he is expected to diagnose his pain on a subjective scale. First, pain is subjective. My pain is very different from your pain. As a redhead, I have increased sensitivity to pain. All pain is relative. Remove a bandaid from my grandson’s leg and he will scream bloody murder, saying, “doctor, it’s a ten!” To my grandson, his pain is very real, but he has no real-world experience with actual pain. Grandpa has sixty-six years of experience with pain — horrible, debilitating pain. I have had tests that were painful; procedures that have left me in tears. Polly gave birth to six children. She understands pain. Three years ago, she had major abdominal surgery and spent twenty-one days in the hospital. Again, lots of pain.
I have had family and blog readers minimize my pain. They believe if I can walk or stand, I must not be in pain. Never mind the fact that walking and standing require psychological and physical contortions from me. One look at my face will tell you everything you need to know. But, people don’t make eye contact much these days. We no longer read body language. If they see me getting out of the car or walking in the store, they assume I must be fine. I’m not fine. And I am never, ever going to be “fine” again. Life for me is pain and endurance; of wondering whether I want to keep living,
Second, people with chronic pain quickly learn that if you tell a doctor nine or ten for your pain level, he will automatically think you are a drug addict looking to score some narcotics. Tell the doctor one, two, or three, he will wonder why you are there. So, I typically say five or six. Bullshit numbers; meaningless numbers, but there ya go doc, you have a number you can input in your digital records program.
Third, I can’t tell you the last time I had a doctor sit down with me and comprehensively talk to me about my pain. Where? How severe? What makes it worse? Do medications help? What physical activities are you able to do, not do? How does your pain affect your sleep; your sex life? Of course, doctors don’t have time to interact with patients this way, especially primary care physicians. They have patients scheduled every 15-20 minutes. No time for personal connection and investigation.
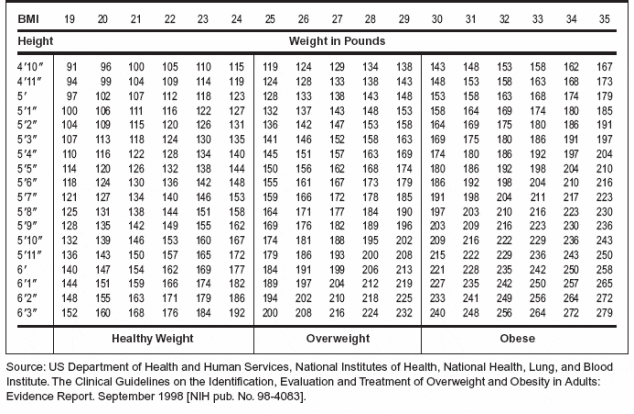
Weight and Body Mass Index (BMI)
I’m obese. The BMI number for me on the doctor’s digital screen is a blinking red number with an exclamation point. This tells the doctor that his patient is fat, as if his eyes couldn’t tell him that already. According to the BMI chart, my “healthy” weight is 140-170 pounds. I weighed 160 pounds at age eighteen; 180 pounds at age twenty-one; 225 pounds at age twenty-five. Was I obese at 225 pounds? Is that even a relevant question? At age twenty-five, I was physically fit. I played basketball and softball. I hunted, hiked, and fished. I cut wood in the fall. I was a physically strong man, yet according to the BMI chart, I was obese.
The BMI number says nothing about the fitness of a person. Most NFL players are obese. Are they unfit? Of course not. I have a big frame. I lost 100 pounds over the past three years, yet I look the “same.” Why? I don’t have a beer belly or ass. I’m built like a fireplug. Certainly, I knew I had lost weight. I dropped two shirt sizes and eight inches in my waist. Yet, to the casual observer or inattentive doctor, I look just like I always have — fat.
Squeeze My Hand
When doctors want to check my strength, they ask me to squeeze their hand. Without fail, they will tell me “Good. You are strong.” My complaints about weakness and debility are dismissed, all because I passed a subjective hand squeeze test.
How does this test tell doctors about the level of my strength? First, isn’t the doctor judging my strength based on his subjective measurement of strength? Second, shouldn’t the measurement of strength be based on how strong or weak I was in the past? Using that criterion, I have lost over half of my physical strength. Sure, I can still squeeze your hand, doc, but there was a day when I could have broken your fingers.
Temperature
“Normal” body temperature is 98.6 degrees, patients are told. That’s what mine was for the first thirty-four years of my life. And then, I contracted mononucleosis and almost died. Mono can be deadly for adults. Afterward, my “normal” body temperature dropped to 97.0 degrees. And thus began a never-ending fight with nurses and doctors about my body temperature. “Doc, I have a fever.” “Your temp is only 99.0. It’s normal.” But . . . he’s already stopped listening. I can’t have a fever, in his mind, because 98.6 is the standard. He doesn’t believe me when I explain mono changed my body temperature. Dare to object and his notes will say, “difficult patient.” And since every other doctor in the practice can see his note, soon the other doctors you see will deem you a “difficult patient.”
Blood Pressure and Glucose Levels
While these numbers can be helpful in diagnosing and treating a patient, they are only a snapshot of a moment in time. Typically, my blood pressure and glucose levels are normal, even exceptional. I get a star by my name for 120/80 and 90 blood sugar level. But, do these numbers tell the whole story about my health? Of course not. I have landed in the ER twice with sky-high blood pressure for no known reason. I have had several instances where I woke up in the night, only to find my blood sugar level was 48 and 50 respectively. Not good. Again, no explanation for the low numbers.
I stopped checking my BP and glucose levels every day. I found the varying numbers too stressful. Occasionally, I will check my numbers, but I typically leave it to my body to tell me what’s up or down, especially my blood sugar levels.
Advice to Doctors
Stop typing. Look your patient in the eye and let him know you care. Ask lots of questions. Pay attention to what his body language is telling you. Use your gifted hands to touch and probe, interacting with the patient all the while. See him as a fellow human being. Never forget, you will be in his shoes one day.
Of course, doing these things takes time, and therein is your problem. Corporate medicine demands efficiency, treating patients like they are line entries on a spreadsheet. The bottom line is more important than the welfare of your patients. Surely, this is not why you got into medicine.
Several years ago, I wrote about a doctor named Bill Fiorini. He’s the kind of doctor I’m talking about. You can read this post here.
Bruce Gerencser, 66, lives in rural Northwest Ohio with his wife of 45 years. He and his wife have six grown children and thirteen grandchildren. Bruce pastored Evangelical churches for twenty-five years in Ohio, Texas, and Michigan. Bruce left the ministry in 2005, and in 2008 he left Christianity. Bruce is now a humanist and an atheist.
Connect with me on social media:
Your comments are welcome and appreciated. All first-time comments are moderated. Please read the commenting rules before commenting.
You can email Bruce via the Contact Form.

Like everything else in society, speed and multitasking are a priority. Nevermind that the work is sub par. Healthcare is a business, and we are products on the assembly line.
Missimontana—Every time I see “ability to multitask “ in a list of job qualifications, I have to wonder whether the employer wants good work.
Bruce—Thankfully, I have not had nearly as much experience with physical pain as you have. But what you say sounds a lot like my experience with depression. People, including some mental health professionals, assume that you’re not depressed if you’re waking up, going to work/school, helping people and laughing at their jokes.
I recently met one of my new primary care providers. I’m with the same health system as always, but I’ll meet my 4th new provider in 3 years in a few months, all because of the high turnover. All were NPs or PAs, who eventually left the hospital system. They’re treated like employees, working for a salary. Anyway, on to my point. They generally give good care and have a little more time than MDs to spend with the patient. But this most recent one astounded me. She never touched the computer while with me. She had reviewed my record before entering the room, and entered her charting after leaving the room. She was so awesome. She looked at me the whole time we talked. It didn’t take any longer than the others, but I felt more heard than before. Her follow up questions to my answers made sense instead of feeling like a checklist. Sadly, she too is moving on.
That doctor is worth keeping! Polly’s ob-gyn is like that. Young doctors need to be taught the importance of human connection.
My doctor fat-shamed me at my last visit, using the ridiculous BMI marker as the reason. I am a 53-year-old competitive obstacle racer who is going through perimenopausal changes, and my 30-something doctor saw fit to tell me that my BMI is almost in the “overweight” category. I chewed her out – I reminded her of my athletic background and that I cannot possibly work out more without risking injury. Besides, I could probably put her on my back and do a squat. I asked her what she thinks I should do, and she had no answer for that. All my health markers are great. So….some stupid chart that has exactly zero to do with how hydrated my body was that day, or how much muscle mass I have, or whether I had pooped yet (sorry) has me at almost overweight? And don’t get me started on the history of the BMI chart…..
I have epilepsy (among other things) which is mostly controlled by anti-seizure drugs and a “chip” from Neuropace installed in my brain (this of course requires surgery) which observes and sends small electric shocks if necessary.. I use an electro-magnetic “wand” to move the data from my chip to a special PC which then sends the data to Neuropace. For me this is great because I worked in IT (database programming) so for me nothing can happen without data.
HOWEVER Kaiser Permanente has a contract with retirement system I retired under. Now they charge me $400 for appointments with my neurologist. Many neurologists have come and gone because they are treated better by other employers. I also pay them $1100 per month in premiums.
I have lost weight recently because the dose of one of my anti-seizure drugs was lowered and now I have less appetite. HOWEVER I m still “overweight”.
Thank you for letting me tell a part of my medical story..